How do urinary tract infections ( UTIs) develop?
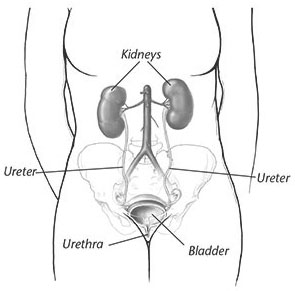
Women are more likely than men to get UTIs because the urethra is shorter in a woman than in a man. In women, the bacteria can reach the bladder more easily.
What causes UTIs?
Women’s anatomy makes them prone to getting UTIs after having sex. The opening of the urethra is in front of the vagina. During sex, bacteria near the vagina can get into the urethra from contact with the penis, fingers, or devices.
Urinary tract infections also tend to occur in women when they begin having sex or have it more often. Using spermicides or a diaphragm also can cause more frequent UTIs.
Infections also can occur when the bladder does not empty completely. This condition may be caused by
- blockage (a stone) in the ureters, kidneys, or bladder that prevents the flow of urine through the urinary tract
- a narrowed tube (or a kink) in the urinary tract
- problems with the pelvic muscles or nerves
What other factors increase the risk of getting a UTI?
You are more likely to get an infection if you
- have had a UTI before
- have had several children
- have diabetes
- are obese
Menopause also increases the risk of getting a UTI. During menopause, the level of estrogen decreases. This decrease can cause changes in the tissues around the urethra that can lead to a UTI.
UTIs can occur during pregnancy. If you are pregnant and think you may have a UTI, be sure to tell your health care provider promptly. If untreated, it may cause problems for you and your baby.
Click on the FAQs below to expand
What are the signs of a UTI?
One sign is a strong urge to urinate that cannot be delayed (urgency). As urine flows, a sharp pain or burning, called dysuria, is felt in the urethra. The urge to urinate then returns minutes later (frequency). Soreness may be felt in the lower abdomen, in the back, or in the sides.
Other signs may show up in the urine. It may
- have a strong odor
- look cloudy
- sometimes be tinged with blood
Blood in the urine may be caused by a UTI, but it also may be caused by other problems. Tell your health care provider promptly if you see blood in your urine.
If the bacteria enter the ureters and spread to the kidneys, symptoms also may include
- back pain
- chills
- fever
- nausea
- vomiting
If you have any of these symptoms, tell your health care provider right away. Kidney infections are serious. They need to be treated promptly.
Symptoms linked with a UTI, such as painful urination, can be caused by other problems (such as an infection of the vagina or vulva). Tests may be needed to confirm the diagnosis. Be sure to let your health care provider know if you have any of these symptoms.
How are UTIs diagnosed?
Your health care provider may first do a simple test, called urinalysis, to find out whether you have a UTI. For this test, you will be asked to provide a urine sample. This sample will be studied in a lab for the presence of white and red blood cells and bacteria. Normal urine should not have bacteria or blood cells in it. If either of these shows up in the urine, you may have a UTI.
The urine sample also may be grown in a culture (a substance that promotes the growth of bacteria) to see which bacteria are present. The sample also may be tested with different antibiotics to see which one destroys the bacteria best. This is called a sensitivity test.
How are UTIs treated?
Antibiotics are used to treat UTIs. The type, dose, and length of the antibiotic treatment depend on the type of bacteria causing the infection and on your medical history.
Treatment is usually quick and effective. Most symptoms go away in 1–2 days. Be sure to take all the medication even though your symptoms may go away before you finish your prescription. If you stop treatment early, the infection may still be present or it could come back after a short time.
For more severe infections, such as a kidney infection, you may need to stay in the hospital. These infections take longer to treat and you may be given medication intravenously (through a tube in a vein).
What is a recurrent infection?
If you have more than two UTIs in a year, you have a recurrent infection. The first step in treatment is finding the cause. Factors that increase the risk of recurrent infection are
- frequent sex
- young age at first UTI
- spermicide use
- diaphragm use
- a new sexual partner
Recurrent infections are treated with antibiotics. A week or two after you finish treatment, a urine test may be done to see if the infection is cured. Changing your birth control method also may be recommended. If you often get UTIs through sexual activity, you may be given an antibiotic to take in single doses after you have sex.
How can UTIs be prevented?
There are a number of ways to prevent UTIs:
- After a bowel movement or after urinating, wipe from front to back.
- Wash the skin around the anus and the genital area.
- Avoid using douches, powder, and deodorant sprays.
- Drink plenty of fluids (including water) to flush bacteria out of your urinary system.
- Empty your bladder as soon as you feel the urge or about every 2–3 hours.
- Try to empty your bladder before and after sex.
- Wear underwear with a cotton crotch.
Unsweetened cranberry juice and cranberry pills may decrease the risk of getting a UTI. The exact amount of juice or pills needed and how long you need to take them to prevent infection are being studied. Treatment with an estrogen cream or pills is being studied as a way to prevent UTIs in women past menopause.
Glossary
Antibiotics: Drugs that treat infections.
Anus: The opening of the rectum on the outside of the body.
Bladder: A muscular organ in which urine is stored.
Dysuria: Pain during urination.
Estrogen: A female hormone produced in the ovaries.
Kidneys: Two organs that cleanse the blood, removing liquid wastes.
Menopause: The process in a woman’s life when ovaries stop functioning and menstruation stops.
Recurrent Infections: Infections that occur more than once, usually within a short time, although they may be spread out over several months.
Spermicides: Chemicals (creams, gels, foams) that inactivate sperm.
Ureters: A pair of tubes, each leading from one of the kidneys to the bladder.
Urethra: A short, narrow tube that carries urine from the bladder out of the body.
Vagina: A tube-like structure surrounded by muscles leading from the uterus to the outside of the body.
Vulva: The external female genital area.
